The pharyngeal reflex, commonly known as the gag reflex, plays a vital role in the body’s defense mechanism. For dental patients, the reflex can sometimes present challenges during treatment. However, patients and dental professionals can work together to ensure a comfortable and safe experience by understanding its function, triggers, and management.
What is the pharyngeal reflex (gag reflex)?
The pharyngeal reflex, commonly known as the gag reflex, is a natural defense mechanism that keeps us safe. It’s designed to prevent choking and expel foreign objects that might accidentally enter the throat. While most of us are familiar with the gagging sensation, few understand how vital this reflex is to our health. This section will explore the basics of the gag reflex, why it’s essential, and how it protects your airway.
The pharyngeal reflex is an involuntary response triggered when certain areas of the mouth and throat are stimulated. This reflex is often associated with the gagging sensation when foreign objects, such as dental instruments, touch-sensitive regions of the throat, soft palate, or tongue.
How does the gag reflex prevent choking?
One of the main functions of the pharyngeal reflex is to prevent choking. When triggered, the reflex causes a contraction of muscles in the throat, helping to expel any foreign objects that may obstruct the airway. This swift muscle contraction protects you from accidentally swallowing or inhaling harmful substances into your lungs.
How does it work with swallowing?
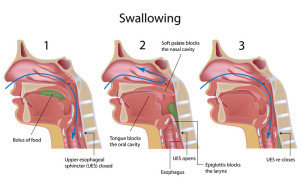
The pharyngeal reflex works closely with the swallowing mechanism, ensuring food and liquids move safely through the esophagus while blocking entry into the windpipe. It’s essential to keep your body safe while eating and drinking and protect against accidental inhalation of foreign objects.
How does it help remove foreign objects from the throat?
In addition to preventing choking, the pharyngeal reflex helps expel any foreign objects that make contact with the back of the mouth or throat. Whether it’s a piece of food or dental instruments during a procedure, this reflex ensures that anything potentially harmful is quickly removed.
How Does the Gag Reflex Work?
At first glance, the gag reflex may seem like a simple reaction, but it’s a complex process involving multiple muscles, nerves, and parts of the brain. This automatic response kicks in when certain areas of the mouth or throat are stimulated. This section breaks down how the gag reflex functions and why it activates when it does, from the involvement of key nerves to the brainstem’s role in controlling the process.
What happens when the muscles in your throat contract?
The pharyngeal reflex is an automatic response that involves the involuntary contraction of throat muscles. When triggered, these muscles react rapidly, causing a gagging or retching response.
What nerves control the gag reflex?
Two critical cranial nerves govern the reflex: the glossopharyngeal nerve (CN IX) and the vagus nerve (CN X). These nerves detect stimulation in the mouth and throat and send signals to the brain, which initiates the reflex response.
How does the brainstem trigger the gag reflex?
The brainstem, particularly the medulla oblongata, coordinates the pharyngeal reflex. Once the glossopharyngeal and vagus nerves detect stimulation, the brainstem processes the signals and activates the appropriate muscles to respond.
How do the soft palate and throat muscles activate?
When the pharyngeal reflex is triggered, the soft palate and throat muscles contract in a coordinated manner, closing off the airway and moving the object or substance away from the throat. This reflexive action protects the airway from obstruction and ensures proper swallowing.
What Triggers the Gag Reflex?
Suppose you’ve ever felt that sudden gagging sensation. What sets it off? The gag reflex can be triggered by various factors, from touching the back of the throat to dental tools or even a nervous response during dental visits. This section explains the common triggers of the gag reflex, how they relate to dental procedures, and why some people are more prone to experiencing it than others.
What causes the gag reflex in the mouth and throat?
The pharyngeal reflex can be triggered by contact with sensitive areas like the soft palate, the back of the tongue, and the throat. This is especially common during dental procedures where instruments may contact these areas.
How do dental procedures and instruments trigger the gag reflex?
Specific dental procedures, such as cleanings or restorations, may involve tools that inadvertently trigger the gag reflex. This can make some patients uncomfortable, but proper management often minimizes the reflex.
Why do dental impressions and X-rays sometimes cause gagging?
Impression trays and x-ray devices used during dental visits can also activate the gag reflex due to their contact with the throat and surrounding areas. Dentists are aware of this potential issue and often take steps to reduce discomfort.
How do anxiety and fear affect the gag reflex?
Patients who experience anxiety or fear related to dental visits may have an increased sensitivity to the pharyngeal reflex. This is because stress can heighten bodily responses, making the gag reflex more pronounced during treatment.
How can foreign objects, like food or dental tools, trigger the reflex?
In addition to dental tools, everyday objects such as food can trigger the pharyngeal reflex. Even dental equipment, such as suction devices, may unintentionally activate the reflex during treatment.
Why is the Gag Reflex Important in Healthcare?
The gag reflex is more than just a response to foreign objects—it plays a vital role in overall health and safety. In medical and dental settings, the reflex helps prevent choking, and its presence (or absence) can provide critical information about neurological health. In this section, we’ll discuss the gag reflex’s importance in healthcare, particularly during dental care, neurological exams, and the diagnosis of certain conditions.
Protection Against Aspiration and Choking
The pharyngeal reflex is crucial for protecting against aspiration, which occurs when food or liquid enters the lungs. The reflex helps prevent choking and ensures the airway remains clear by triggering an immediate gagging response.
Why is the gag reflex used in neurological exams?
Neurologists often assess the pharyngeal reflex to gauge the health and functionality of the brainstem. A properly functioning gag reflex indicates that the brainstem correctly processes sensory signals and coordinates muscle responses.
How can the gag reflex help diagnose neurological conditions?
Abnormalities in the pharyngeal reflex can also be a sign of neurodegenerative diseases, such as ALS (amyotrophic lateral sclerosis) or Parkinson’s disease. A weakened or exaggerated reflex may point to underlying neurological issues.
Why is managing the gag reflex important in dental care?
The pharyngeal reflex plays a significant role in ensuring patient safety in the dental setting. Dentists carefully manage the gag reflex to prevent choking or aspiration during procedures that involve the mouth and throat.
Why Do Some People Have a Stronger Gag Reflex?
Not everyone experiences the gag reflex in the same way. Some people have a hypersensitive reflex that can be easily triggered, while others barely notice theirs. What causes these differences? This section delves into the factors influencing gag reflex sensitivity, from age to medical conditions. It explores why specific individuals may struggle more with an overactive reflex, especially in a dental setting.
Hypersensitive gag reflex (increased response)
Some individuals have a hypersensitive gag reflex, where minimal contact with the throat or soft palate triggers a strong reaction. This can be challenging during dental procedures but can be managed with various techniques.
Reduced or Absent Reflex in Some Individuals
Conversely, some people have a reduced or absent gag reflex. This can occur due to age, neurological conditions, or other medical factors. While a reduced reflex may seem beneficial during dental treatments, it also reduces the body’s ability to protect the airway.
Influence of Age and Medical Conditions on Sensitivity
Age and certain medical conditions can affect the sensitivity of the pharyngeal reflex. Older adults may experience diminished reflexes, while individuals with specific neurological conditions may have heightened sensitivity.
Managing Overactive Reflexes During Dental Visits
Dentists can use desensitization techniques, local anesthetics, or relaxation exercises to minimize discomfort during procedures for patients with an overactive gag reflex.
What Happens When the Gag Reflex Becomes a Problem?
For some, the gag reflex can be more than just a protective mechanism—it can become a source of discomfort or even a barrier to necessary medical or dental care. In hyperactive reflexes, patients may experience difficulty during procedures, while those with a reduced reflex may face other risks. Here, we’ll look at the common disorders related to the pharyngeal reflex and discuss how they can impact dental treatments and overall health.
What is a hyperactive gag reflex, and why is it common in dental patients?
A hyperactive gag reflex is common among dental patients and can make treatments more challenging. However, with proper management, the reflex can be controlled to ensure a smoother experience.
Dysphagia (Swallowing Difficulties)
Dysphagia, or difficulty swallowing, can sometimes be linked to an abnormal pharyngeal reflex. This issue requires careful evaluation to prevent complications during eating and drinking.
What happens if the nerves controlling the gag reflex are damaged?
Damage to the glossopharyngeal or vagus nerve can impair the pharyngeal reflex, reducing the ability to protect the airway from foreign objects.
How do conditions affecting the brainstem impact the gag reflex?
Conditions that affect the brainstem, such as stroke or ALS, can disrupt the coordination of the pharyngeal reflex, making it less effective in protecting against choking or aspiration.
How is the Gag Reflex Tested?
Medical and dental professionals often need to assess the gag reflex to ensure it’s functioning correctly. This simple test stimulates specific mouth and throat areas to observe the reflex’s response. In this section, we’ll explore the different methods used to test the gag reflex and how these tests can provide insight into a patient’s health, especially about the brainstem and nervous system.
Visual Inspection and Stimulation of the Soft Palate
One method for testing the pharyngeal reflex involves visually inspecting the mouth and stimulating the soft palate. Dentists or healthcare professionals may use a tongue depressor to gently touch the soft palate or back of the throat, which typically triggers the reflex. This helps assess the reflex’s strength and functionality.
Use of Tongue Depressor During Oral Exams
A tongue depressor is a common technique for evaluating the pharyngeal reflex. Professionals can gauge how quickly and strongly the reflex is activated by pressing down on the tongue and causing contact with the back of the mouth.
Neurological Assessments Focusing on the Reflex Arc
In some cases, a thorough neurological exam is necessary to assess the pharyngeal reflex, especially if there are concerns about brainstem function or nerve damage. These assessments focus on the entire reflex arc—from the stimulation of sensory receptors to the coordination of muscles by the brainstem.
Tests During Dental Treatments to Gauge Sensitivity
Dentists may perform tests to determine a patient’s gag reflex sensitivity during dental treatments. This helps them tailor their approach, using techniques that minimize discomfort and ensure the reflex doesn’t interfere with the procedure.
How Can You Manage an Overactive Gag Reflex?
An overactive gag reflex can make dental visits stressful, but fortunately, there are several ways to manage it. From desensitization techniques to local anesthetics, healthcare providers can use a variety of approaches to help patients feel more comfortable. This section explores different strategies for controlling an overactive gag reflex during dental procedures, including behavioral therapies, relaxation techniques, and medical interventions.
Desensitization Techniques for Dental Patients
Desensitization techniques can be effective for patients with a hyperactive gag reflex. These techniques involve gradually exposing the sensitive areas of the throat or palate to gentle contact, allowing the body to become accustomed to the sensation over time. These techniques are instrumental in reducing discomfort during dental procedures.
Behavioral Therapy to Reduce Reflex Activation
In some cases, behavioral therapy may help patients learn to control their gag reflexes. This approach focuses on relaxation techniques, breathing exercises, and cognitive strategies to help reduce the reflex response during stressful or anxiety-inducing situations, such as dental visits.
Use of Local Anesthetics During Dental Procedures
Local anesthetics can temporarily numb sensitive areas of the mouth, reducing the likelihood of triggering the gag reflex. Dentists often apply a numbing spray or gel to the soft palate or throat before performing procedures that activate the reflex.
Relaxation and Breathing Techniques to Manage Anxiety
Patients who experience anxiety during dental treatments may benefit from relaxation and breathing techniques. Controlled breathing can help calm the body’s natural reflexes and reduce the likelihood of gagging. Dentists may also recommend mindfulness practices to help patients stay relaxed during appointments.
Medications that Reduce Hyperactivity in Severe Cases
In cases where the gag reflex is extremely sensitive and other treatments are not effective, medications may be prescribed. These medications work by calming the nervous system or numbing the area, helping to control the reflex response during dental procedures.
What Parts of the Nervous System Control the Gag Reflex?
The gag reflex doesn’t happen in isolation—a network of nerves and brain pathways controls it. Specifically, the glossopharyngeal and vagus nerves detect stimulation in the mouth and throat, while the brainstem coordinates the reflex action. In this section, we’ll explore the neurological pathways that control the gag reflex and discuss how damage to these systems can affect its function.
Which cranial nerves are responsible for the gag reflex?
The glossopharyngeal nerve (cranial nerve IX) and the vagus nerve (cranial nerve X) are the primary nerves responsible for the pharyngeal reflex. These nerves detect stimulation in the throat and send signals to the brainstem, activating the muscles accountable for the gagging response.
How does the medulla oblongata control the reflex?
The medulla oblongata, located in the lowermost part of the brainstem, plays a crucial role in coordinating the pharyngeal reflex. Once the glossopharyngeal and vagus nerves detect stimulation, the medulla processes the information and triggers the muscle contractions that create the reflex.
What role do sensory receptors in the throat play in the gag reflex?
The sensory receptors in the soft palate and oropharynx (the part of the throat just behind the mouth) are susceptible to touch. When activated, they send signals through the cranial nerves to initiate the gag reflex, ensuring foreign objects are quickly expelled.
How do neurological conditions affect the reflex pathways?
Neurological diseases that affect the glossopharyngeal or vagus nerves or the medulla oblongata can interfere with the proper functioning of the pharyngeal reflex. Conditions like ALS, stroke, or multiple sclerosis can damage these pathways, leading to an impaired reflex and increasing the risk of choking or aspiration.
How Does the Gag Reflex Change as We Age?
The gag reflex evolves throughout our lives, from infancy to old age. Young children often have a more sensitive reflex, while the elderly may experience a weakened or absent gag reflex. These changes can impact how dental and medical treatments are approached. In this final section, we’ll explore how the gag reflex develops in different age groups, the challenges in pediatric and elderly care, and what dentists can do to manage the reflex across all ages.
Reflex Development in Infants and Children
The pharyngeal reflex is present from birth and is a vital protective mechanism in infants and children. However, it can be more sensitive in young children, as their nervous systems are still developing. This sensitivity can sometimes cause challenges during dental visits, but dentists are experienced in managing this reflex in pediatric patients.
Changes in Reflex Sensitivity with Age
As individuals age, the sensitivity of the pharyngeal reflex may decrease. Elderly patients may have a weakened or absent gag reflex, which can increase the risk of choking. Dental professionals consider this when treating older patients to ensure their safety during procedures.
Considerations for Elderly Patients During Dental Treatments
For elderly patients with reduced reflex sensitivity, dentists may adjust their approach to minimize the risk of choking or aspiration during procedures. This might involve using smaller instruments or positioning the patient to reduce the likelihood of gagging.
Managing Gag Reflex in Pediatric Dental Care
In pediatric dental care, managing the gag reflex is a priority. Dentists use distraction, positive reinforcement, and desensitization techniques to help children feel more comfortable during procedures. This helps ensure the dental experience is positive and stress-free for young patients.
Conclusion
By understanding the pharyngeal reflex and its role in dental care, patients and dentists can take proactive steps to manage it effectively. Whether through desensitization techniques, relaxation methods, or local anesthetics, there are many ways to ensure that dental procedures remain comfortable while maintaining the body’s natural defenses.
We prioritize patient comfort and safety at PV Smiles in Scottsdale, AZ, offering tailored solutions for those with an overactive gag reflex. Our experienced team is dedicated to providing gentle, compassionate care and ensuring that every visit is as stress-free as possible.
Contact PV Smiles today to schedule a consultation if you’ve been avoiding dental care due to discomfort or a strong gag reflex. Let us help you maintain your dental health without anxiety and enjoy a more comfortable experience at the dentist.